What is Personal Protective Equipment?
PPE (Personal Protective Equipment) keeps you safe from blood, hazardous materials, and OPIM.
PPE includes:
- Face shields
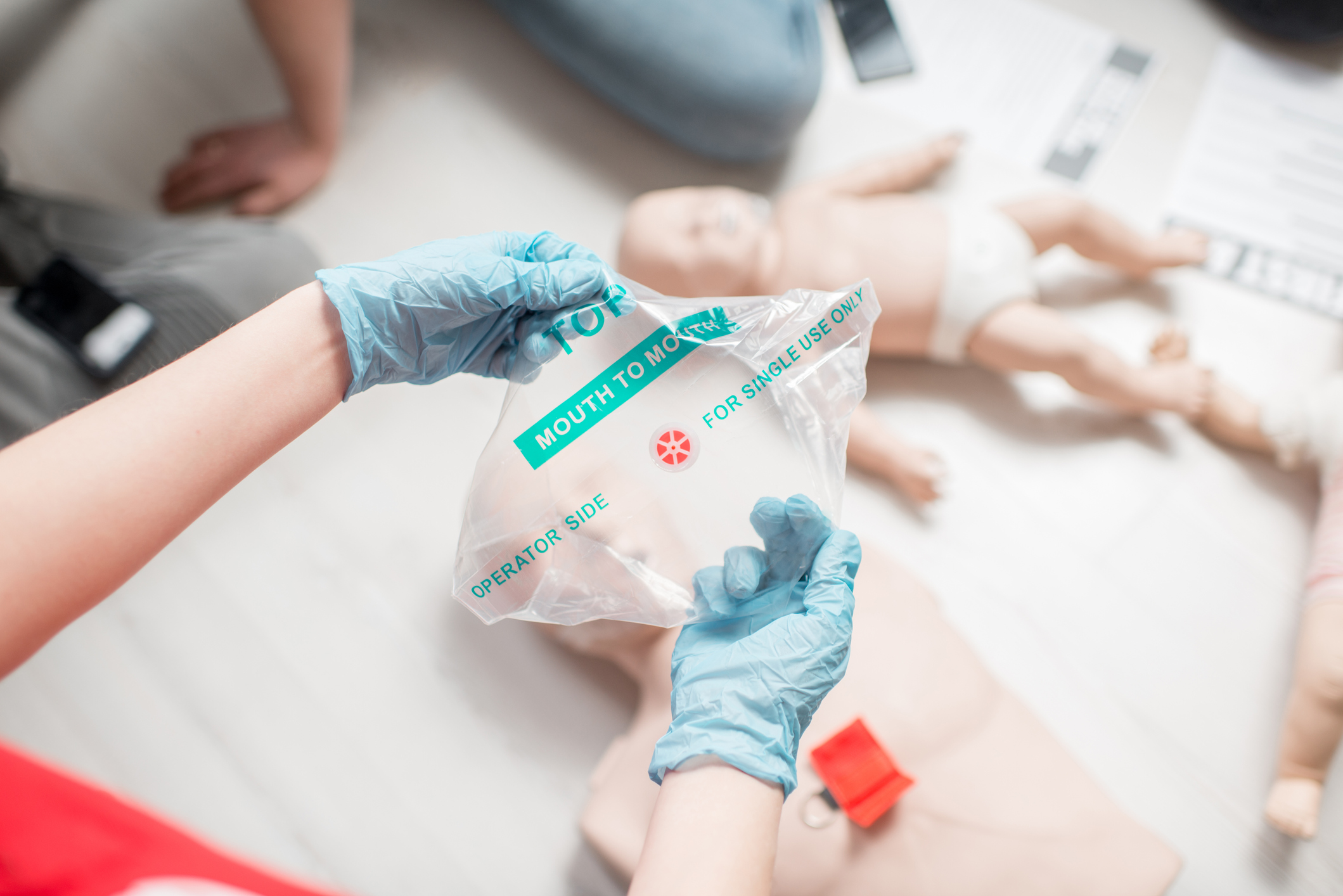
- CPR shields
- Gloves
- Goggles
- Gowns
- Masks
If and when required, employees must wear these protective garments whenever they anticipate any likelihood of exposure. Additionally, employees should wear surgical caps or hoods and shoe covers/boots in instances when gross contamination can reasonably be anticipated.
All Personal Protective Equipment promotes safety by creating a barrier between you and the infection/hazardous materials. Before arriving at the scene of the accident, you must assess the situation to determine the risks and to use the proper PPE.
PPE must be selected appropriately for each unique task and must be readily accessible for all employees. In extraordinary and rare cases an employee may temporarily and briefly forego the use of PPE. If this occurs, the employer must document and investigate such a situation thoroughly to determine how to prevent it further down the line. If an employee is allergic to any PPE item, the employer is required to provide an alternative. Employers must also be sure that all employees are familiar with the types of equipment they'll use before engaging or handling hazardous materials, OPIM or blood.
PPE examples include CPR shields provide protection against exposure when performing CPR. Face shields provide splash and high impact protection, while gloves protect against exposure from skin contact with chemicals, infectious agents, cold, heat, and cutting objects. For proper protection, be sure to use the correct hand.
Goggles are designed to reduce the risk of exposure to laser radiation, chemical splashes, or flying debris. Gowns are used to prevent the penetration of infectious blood, hazardous materials, or other OPIM. Masks are used to protect the employee from airborne materials or liquid contaminating the face.
How to clean and decontaminate PPE
Employees responsible for cleaning surfaces that could be contaminated with bloodborne pathogens must be protected from exposure. Employers are tasked with ensuring that workers are protected from said exposure and that they are not exposed to harmful levels of chemicals used for disinfection or cleaning.
What are the guidelines?
Any visible surface contaminated with blood, urine, faeces, vomit, or other body fluids must be immediately cleaned and disinfected. Isolate any areas of suspected contamination until the decontamination process is complete to reduce the risk of exposure to individuals who are not carrying out the work. All bulk spill matter or visible contamination must be treated with an appropriate disinfectant before any clean up or the removal of bulk material begins. After disinfecting and disposing of the bulk material, use a disinfectant to decontaminate and clean the area.
Any spills should be covered with an absorbent material. Then, a disinfectant should be applied to saturate the area and soak into the spills. This will allow the bleach to kill any infectious agent or virus that could be present. When using disinfectant, ensure adequate ventilation by opening windows and doors or using appropriate ventilation equipment. If chemical disinfectants are used, an employer may have to train workers on how to protect themselves against chemical hazards.
How to use disinfectants
To disinfect surfaces after bulk spill material has been removed or to treat contamination, use an EPA-registered disinfectant suitable for non-enveloped viruses. If commercial disinfectant products are not available, household bleach or other disinfectants are suitable alternatives. Use a 1:10 solution of bleach to water and mix the chemicals together before use. Note: certain combinations can be deadly or reduce the disinfectant's effectiveness.
When to use respiratory protection
If workers are exposed to bio-aerosols suspected of or known to contain OPIM, blood and other hazardous materials, respiratory protection is necessary. In these situations, medically qualified employees must use a fit-tested N95 respirator (NIOSH-approved) at a minimum.
How to clean equipment
An employer must choose Personal Protective Equipment (PPE) that will safeguard workers against bloodborne pathogens to which they could be exposed to when cleaning. PPE used for cleaning includes gowns, goggles, gloves, face shields, and face masks. As well as protective leg, sleeve, and fluid-impermeable or fluid-resistant shoe coverings will lower the risk of contact with infectious materials. Respiratory protection may also be required to shield workers from exposure to OPIM, blood, and other hazardous materials.
How to remove PPE
Employees should remove protective clothing before leaving the room, and dispose of it in an appropriately designated area or container for washing, storage, disposal or decontamination. Once the disinfection and cleaning processes are complete, remove all PPE and wash your hands with soap and water. Use an alcohol-based hand gel if there's no access to clean, running water.
How to properly dispose of waste
Any PPE or materials used during cleanup and decontamination need to be soaked in disinfectant. Once soaked, double-bag them and place the gear in a leak-proof container to minimize further risk of exposure. If there are sharps, use a puncture-proof container. If you have to dispose of contaminated objects which have porous surfaces that can't be disinfected, follow all regulations and guidelines for correct disposal.
Wash hands corrrectly
This part of the plan should describe your guidelines for hand-washing. These procedures should include a provision for workers to wash their hands as soon as possible after blood comes into contact with their eyes, skin, or mucous membranes. This must be carried out after PPE or gloves have been removed.
If running water is not available, your hand-washing plan must outline what alternatives your workers must use to clean their hands, such as disinfectant towels or hand sanitizers. In emergency situations at remote sites, employees must wash their hands under running water as soon as they are able.
How to flush eyes or mouth
If your eyes are splattered with blood or OPIM, immediately flush with water or saline eyewash for 5-10 minutes; if splashed in your mouth or on your face, rinse with water for 5-10 minutes.
How to decontaminate equipment
To ensure those involved in the handling, transportation and repair of equipment are not exposed to infectious materials, all equipment must be decontaminated before being repaired or shipped. Here, your procedures should outline the steps to follow to clean equipment before it is handled by someone else. This might include instructions for disassembly to allow internal components to be decontaminated.
If full decontamination cannot be carried out, you will need to attach a label displaying a biohazard warning. You will also be required to indicate which portions of the equipment are still contaminated. You are free to choose the labeling method you use, but self-adhesive labels, string tags, and sheets of paper are all acceptable.
How to handle specimens
If your employees will handle specimens, you will need to identify and outline the best work practices for proper handling. This could include describing the appropriate methods for packaging specimen containers for shipping. If you don't handle specimens, you don't need to complete this section.
How to handle sharps
Needles should never be recapped or bent by hand unless absolutely necessary, and your procedures should require that all sharps are placed in puncture-resistant containers which are easily identifiable. Also, these containers must be located as close as possible to where sharps are likely to be found or used, such as hospital laundries.
Your decisions regarding the disposal of sharps must be supported by sound professional judgment. For example, you may decide to place containers in each examining room where a needle is used. Sharps with engineered injury protection must also be placed in the appropriate container once they've been used.